Peripheral Arterial Disease
What Is Peripheral Arterial Disease (PAD)?
Peripheral arterial disease (also called peripheral artery disease or peripheral vascular disease, PVD), is a disease in which blood flow to your limbs is limited due to narrowed or blocked arteries. Over time, our arteries tend to build up a fatty material that can block blood flow completely. As the lower extremities receive less oxygen, muscle groups and tissue below the blockages may suffer lower bloodstream oxygen. Because of this, patients may experience pain or cramping–called claudication. Imagine holding your breath for two minutes, and then imagine that pain being in your foot every time you take a few steps. Along with pain, however, reduced blood flow over time can lead to the formation of wounds, limited ability to heal, gangrene, and eventually limb loss. This is especially pronounced in smokers, diabetics and patients with renal failure.
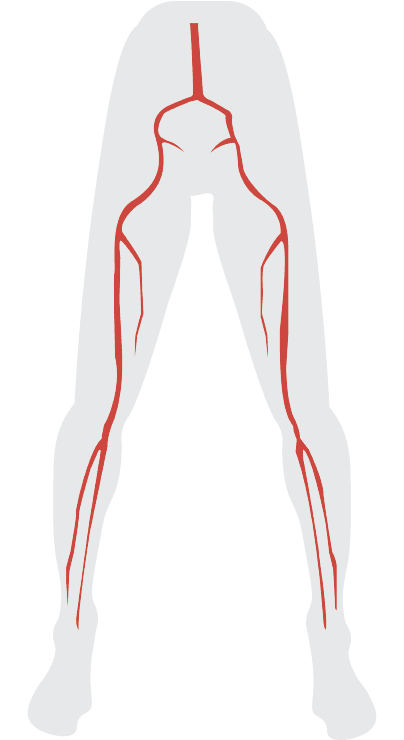
How peripheral arterial disease (PAD) is treated depends on the progression of the disease. When the disease is caught early enough, a few simple lifestyle modifications and continuous vigilance may be the best approach. In this case, one of our vascular specialists may instruct you to introduce some form of exercise into your daily activities, or prescribe medications to:
If you have rest pain or wounds in your feet (particularly if you are a smoker, diabetic or dialysis patient), contact our vascular specialists NOW.
- Lower blood pressure and cholesterol levels,
- Prevent the formation of blood clots that could cause a heart attack or stroke,
- Help reduce pain while walking or climbing stairs.
In addition to these modifications, we will schedule occasional checkups to monitor the progression of the disease.
Unfortunately, most patients aren’t aware of their PAD until it requires some form of intervention. In this case, we may still suggest incorporating exercise and medications, but our attention then shifts to the arteries themselves in order to return blood to the legs. This is done during a safe, minimally invasive procedure called an angiogram; during an angiogram, we enter the arteries through a small incision–typically in the groin, though we may access from other areas depending on your condition and the locations of your blockages–and insert a series of flexible wires and catheters to visualize the vasculature. Through this method, we are able to locate the areas where blood cannot easily pass, and take the appropriate steps to restore blood flow. This is usually done by a combination of atherectomy, angioplasty, and possibly stenting. Angiograms are not long procedures, and the patient is usually able to go home by the end of the day after a short period of recovery in one of our private suites.
What is Critical Limb Ischemia (CLI)?
PAD is often underrecognized and undertreated. Some patients may progress from cramping in their legs while walking, to cramping and pain at rest. Other patients may have no preceding symptoms and still develop this “ischemic rest pain”. In this state, the foot or leg may be in a state of constant, burning pain or numbness, particularly when elevated, and will usually be relieved with the foot put back on the floor (because gravity is able to pull the blood back down into the foot). These patients are in a critical state–their lower limbs are not receiving enough blood even in a resting state. Patients in this category are at significantly higher risk of non-healing wounds, ulceration (hole in the foot), or gangrene (dead or blackened tissue). Unless the underlying disease is managed, many of these people will have an amputation of the affected leg or die of a heart attack or stroke.
If you have rest pain or wounds in your feet (particularly if you are a smoker, diabetic or dialysis patient), contact our vascular specialists NOW.
PAD Causes
Like most diseases, it can be difficult to pinpoint a single, ultimate cause for peripheral arterial disease. Instead, it is typically a combination of genetics, pre-existing illnesses, and lifestyle factors that give way to the buildup of plaque in arterial structures. There are several known risk factors associated with PAD to be aware of:
- Smoking
- Over the age of 50
- High Blood Pressure
- High Cholesterol
- Stroke
- Obesity
- Diabetes
- Chronic Kidney Disease
- Coronary Heart Disease
- Any family history of the above listed ailments.
PAD Symptoms
Again, the symptoms of PAD often go unnoticed by many patients and physicians alike. Here are some things to look out for:
- Pain or tiredness in the calf, thigh, or buttock when walking that is relieved with rest (intermittent claudication).
- Toes or feet that become discolored when upright.
- Leg or foot pain that disturbs your sleep (rest pain).
- Sores or wounds on toes or feet that heal slowly, or not at all.
- Burning feet (often diagnosed as neuropathy) that do not respond to medication.
- Toes that turn black (gangrene).
- Changes in the skin on your leg - color, shiny, hair loss.
See the signs of PAD

Hover to view symptoms
How is PAD diagnosed?
According to the CDC, over 8.5 million people over the age of 40 in the U.S. have PAD. To put that further into perspective, one in every twenty people over the age of 50 have PAD–a massive underestimation, given how frequently the disease goes undiagnosed. Every year, there are over 150,000 amputations in the U.S. Perhaps scarier is the fact that 48% of PAD patients that receive an amputation die within the first year. That figure increases to 71% after three years. Because of this, it is critically important that we, as a nation, become better at recognizing and diagnosing end-stage PAD, called critical limb ischemia (CLI).
PAD diagnosis begins with recognizing the symptoms. Often, our patients experience classic PAD symptoms, but attribute them to aging or another ailment. Others, like diabetics, may remain clinically silent with severe disease until a wound appears. By being mindful of PAD risk factors & symptoms, our patients may be able to better communicate to their physicians what they’ve been experiencing, and the medical diagnosis can begin.
Several diagnostic tests exist for diagnosing and confirming PAD / CLI. Physicians may rely on a simple ankle-brachial index (ABI), where they compare blood pressure readings in the leg and arm, looking for lower readings in the leg, which may indicate blockages are present. To better localize the blockages, your physician may request for a doppler ultrasound–which uses sound waves to help visualize the flow of blood through your arteries. Magnetic resonance angiography (MRA) and computerized tomography angiography (CTA) are also non-invasive ways of imaging the arteries in order to gain an understanding of where blockages may be.
Finally, there is the minimally invasive procedure of angiography, where–by using a series of small catheters and wires–the arteries can be seen live under x-ray, and endovascular intervention can occur on site if disease is found (read more about this in our treatment options). In this case, treatment can occur immediately if there is disease present in the arteries.
PAD Treatment
PAD is a chronic, progressive, and systemic disease. This means that once present, it will not go away completely, regardless of therapy. The goal of treatment is to relieve the pain associated with the disease so that you as a patient can remain active and return closer to your normal lifestyle–and lessen the likelihood of greater complications (like tissue loss or amputation). Treatment type depends largely on the stage of the disease at diagnosis in addition to patient risk factors, but generally follows a pattern:
- Lifestyle modifications. This may include adding in a bit of walking to your daily routine, making changes to your diet, the addition of certain medications, and of course–if you smoke, you should stop.
- Minimally invasive procedures for vascular reconstruction. Click here to learn more about these options.
- Invasive surgical procedures. This can include bypass surgery and amputation*.
*Although we list amputation for the sake of education, we at Palm Vascular Centers do not see amputation alone as a form of treatment for PAD. Amputation may be a life-saving surgery, but we believe should generally be a last-resort, if you as the patient are invested in keeping your limbs attached. Additionally, without proper vascular reconstruction, amputations may not heal and can resort in a vast array of postoperative complications. If you or a loved one have been diagnosed with PAD and are facing amputation, we encourage you to look for another opinion.
Lifestyle Changes
PAD treatment often includes making long-lasting lifestyle changes. If you have PAD, or are aiming to lower your risk, your health care provider may prescribe one or more of the following:
- Quit smoking. Don’t smoke, and if you do, quit. Lower your numbers.
- Work with your health care provider to correct any high blood pressure, cholesterol, and blood glucose levels.
- Follow a healthy eating plan. Choose foods that are low in saturated fat, trans fat, and cholesterol.
- Get moving. Make a commitment to be more physically active. Aim for 30 minutes of moderate-intensity activity on most, preferably all, days of the week.
- Aim for a healthy weight. If you are overweight or obese, work with your health care provider to develop a supervised weight loss plan.
Medication for Peripheral Arterial Disease
In addition to lifestyle modifications, your health care provider may prescribe one or more medications that help:
- Lower high blood pressure and cholesterol levels and treat diabetes
- Prevent the formation of blood clots that could cause a heart attack or stroke
- Help reduce leg pain while walking or climbing stairs
- Peripheral Arterial Disease Clinical Treatments
- For people suffering from Peripheral Arterial Disease (PAD), the buildup of plaque in the arteries of the legs often leads to severe and even debilitating leg pain. When the plaque becomes “calcified,” limited options have been available to successfully treat the problem – until now.
Minimally Invasive Surgical Treatment Options for PAD
Angiograms
Angiograms are minimally invasive diagnostic procedure used to confirm the presence of disease.
Angioplasty
Angioplasty is a common form of treatment in which a balloon is introduced into the blockage and inflated, then allowed to deflate and removed from the vessel. In the process, the balloon expands the arterial wall, re-establishing blood flow.
Stent Placement
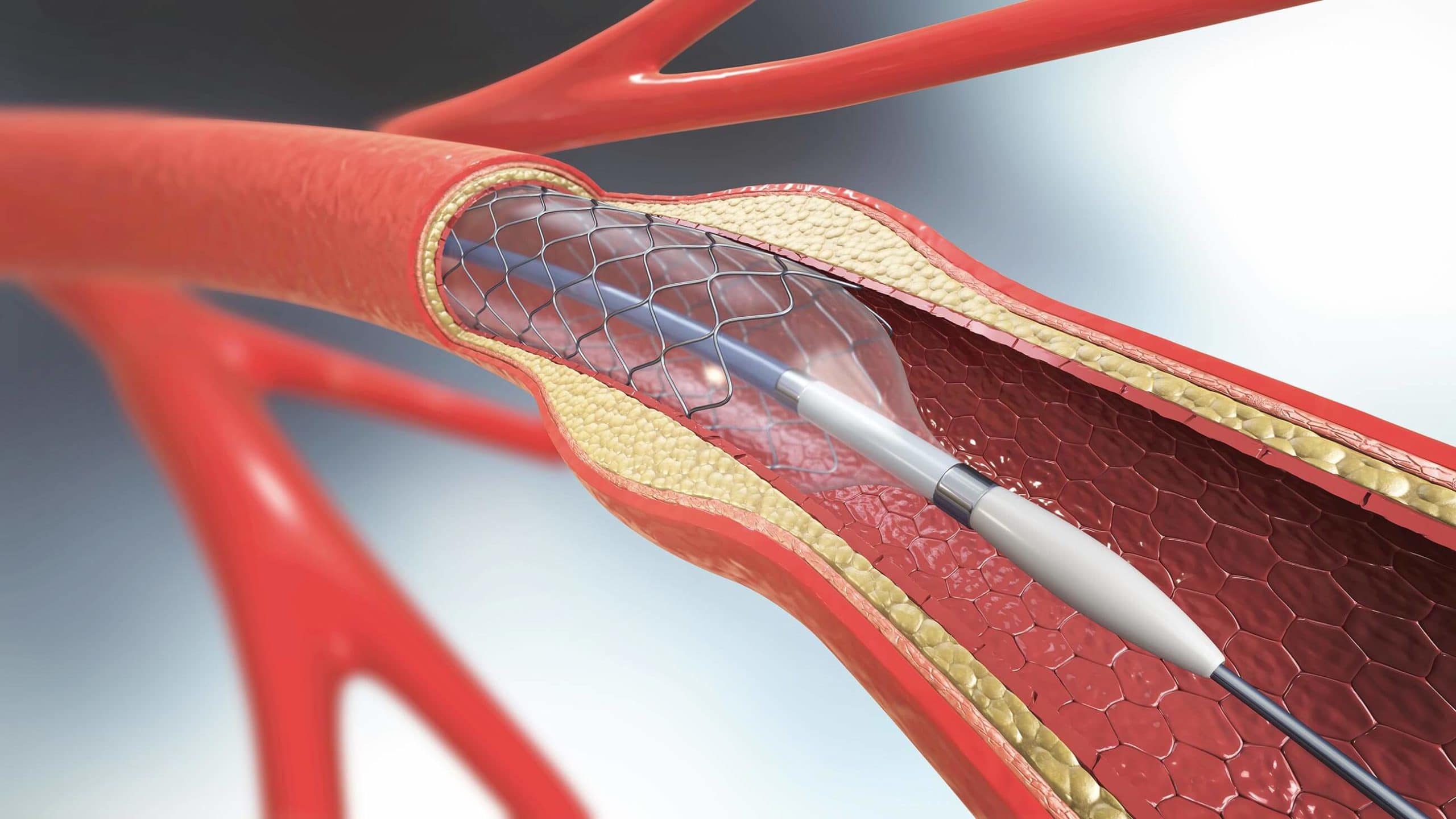
Stents are small tubes made of a metal mesh that can be used to provide backing to the arterial wall, assisting in keeping the artery open. Once put in place, stents remain as permanent structures in the vasculature.
Atherectomy
Atherectomy is the removal of plaque from a blood vessel. There are many different forms of atherectomy, and we vary what form we use depending on the circumstances of the blockage–size, composition, location. Typically, we use laser atherectomy; a superheated laser zaps the plaque away, allowing for blood to flow more easily. In cases where the plaque is heavily calcified, we may opt for orbital atherectomy, where a very small stud is rotated through the plaque, shaving away the hardened blockage and making the artery pliable enough to undergo balloon angioplasty.